Table of Contents Show
Abstract
Alzheimer’s disease (AD) is a progressive neurodegenerative disorder with an alarming and rising prevalence in Nigeria. Artificial Intelligence (AI) offers a promising pathway to support early diagnosis and personalised treatment in the healthcare system. This study proposes the development of a culturally sensitive, AI-powered diagnostic framework tailored to the Nigerian context. Using a mixed-methods approach, 600 participants will be recruited across three groups: diagnosed AD patients (n = 300), healthy controls (n = 200), and individuals at high risk (n = 100) from federal teaching hospitals in southwestern Nigeria. The study will gather multimodal data, including neuroimaging, cognitive assessments, genomics, comorbidities, functional status, lifestyle factors, treatment history, and socio-demographic details, to train and validate interpretable machine learning models aimed at early intervention and personalised treatment. The model will be trained to predict AD risk levels (low, moderate, high) and provide tailored treatment recommendations, including pharmacological options, neuropsychological rehabilitation, caregiver support, and follow-up schedules, based on individual profiles. Primary outcome measures will include diagnostic accuracy (>85%), precision in treatment stratification, and alignment with clinical decision-making. Secondary outcomes will involve provider satisfaction, ease of interpreting the model, and potential for integration into existing healthcare workflows. By ensuring ethical design, clinician readiness, and real-world applicability, this study aims to position AI as a transformative tool in Nigeria’s evolving neurological care landscape.
Keywords: Alzheimer’s disease, Nigerian healthcare, artificial intelligence, machine learning
Introduction
Dementia has quietly become one of the world’s deadliest burdens, ranking as the seventh leading cause of mortality globally. Of all known forms of dementia, Alzheimer’s disease (AD) accounts for approximately 60% (World Health Organisation 2025). In Nigeria, the situation is particularly concerning, with reported AD prevalence increasing by over 400% between 1995 and 2015 (Adeloye et al. 2019). This figure is likely to rise, given our rapidly ageing population, underdiagnosis, and low public awareness.
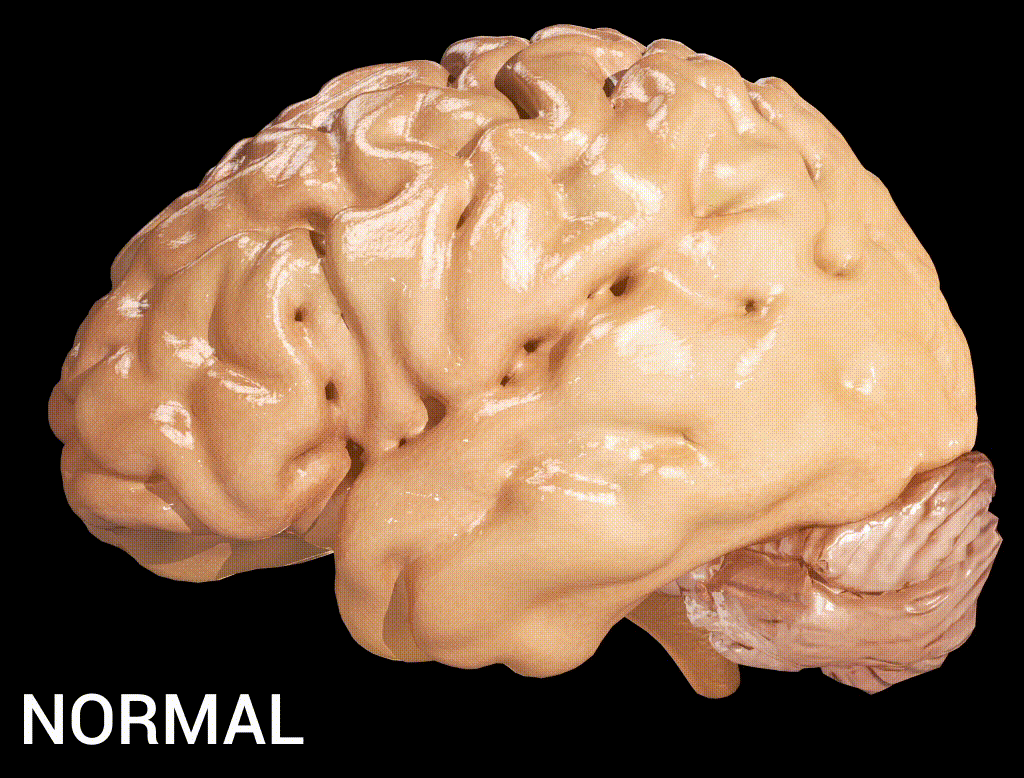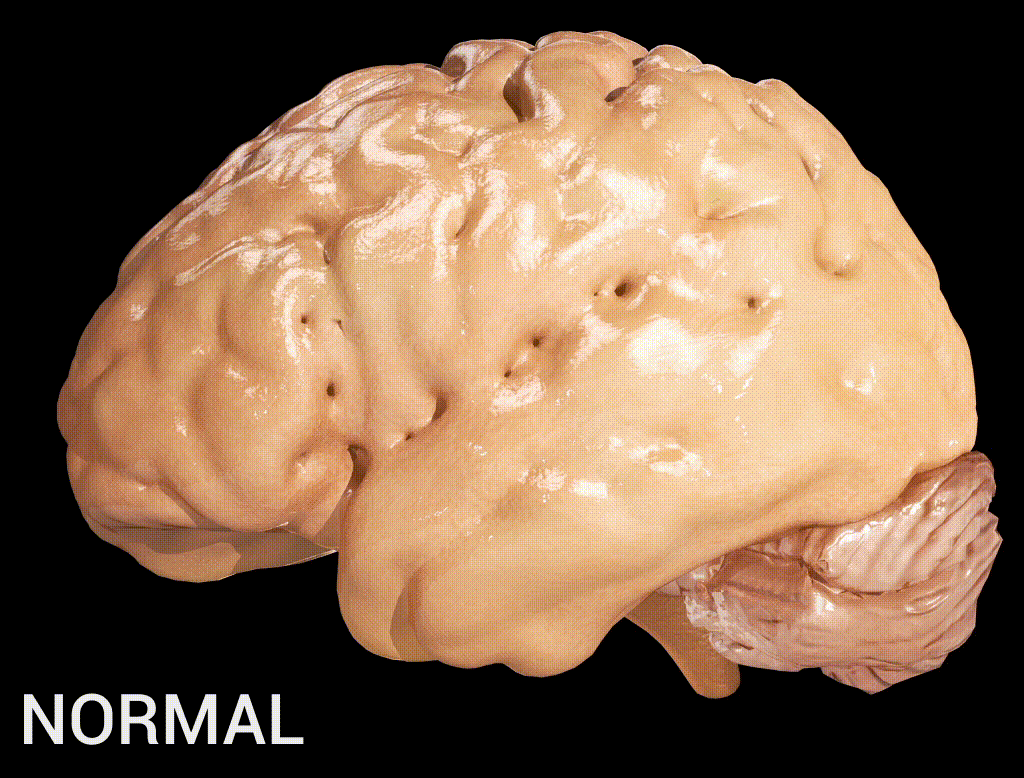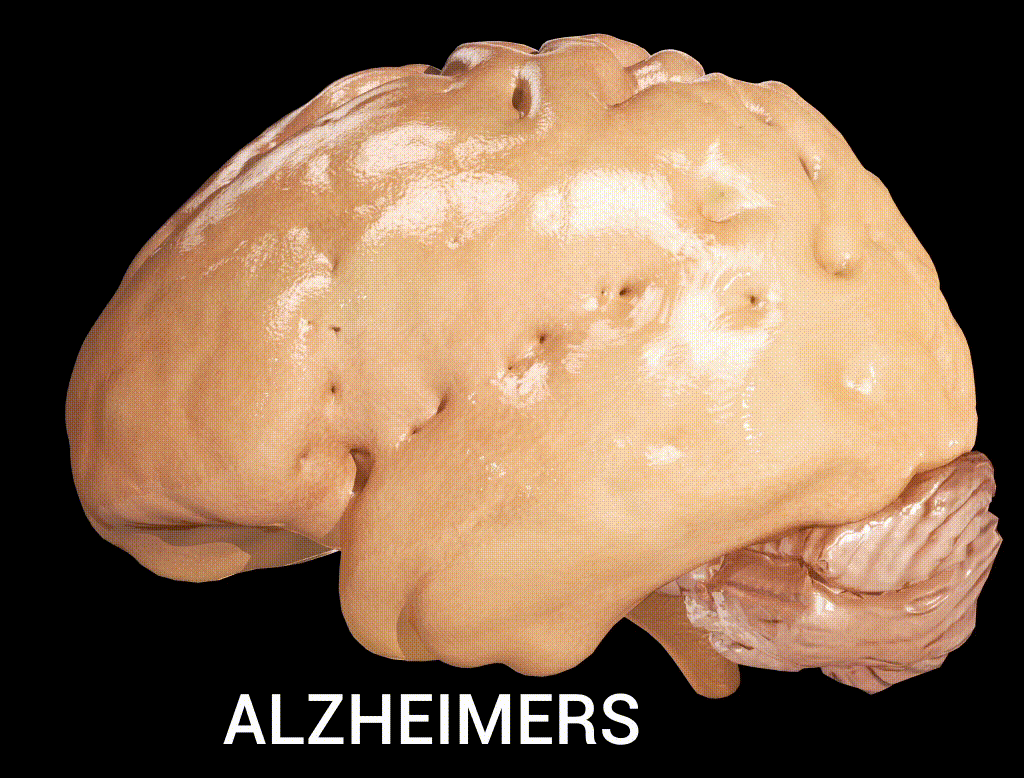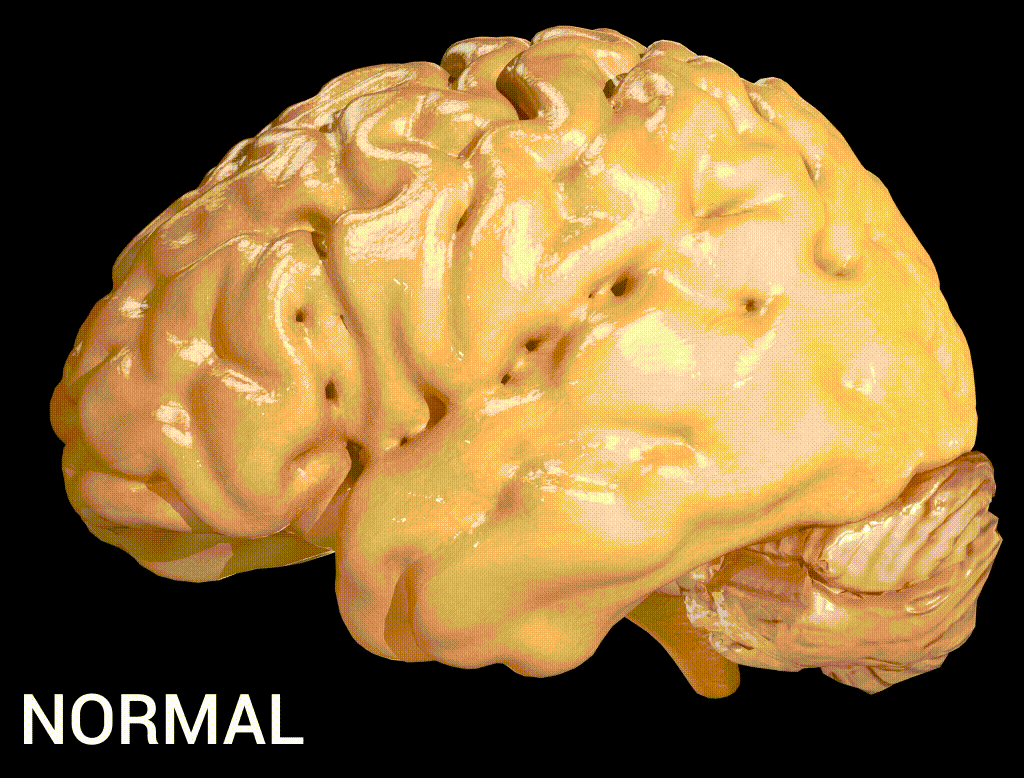
Alzheimer’s disease encompasses more than just memory loss. It is a progressive neurodegenerative condition that impacts cognition, daily functioning, behaviour, and quality of life. The burden is felt by patients, caregivers, families, communities, and the fragile healthcare infrastructure, which struggles to respond meaningfully (Gupta and Iftekhar 2024). Despite extensive global research on early detection and intervention, African nations, such as Nigeria, remain underrepresented in the data and innovations that drive care solutions.
AI presents a unique opportunity to bridge this gap if implemented thoughtfully. On a global scale, AI has demonstrated effectiveness in streamlining diagnostics, analysing intricate biomedical data, predicting disease progression, and improving treatment outcomes across various fields, including neurodegenerative diseases (Rane et al. 2023; Kale et al. 2024). In the context of Alzheimer’s, AI’s capability to integrate cognitive, imaging, genetic, and behavioural data allows it to reveal subtle indicators that might otherwise remain unnoticed in standard clinical practice.
However, this technology has been trained and validated in Western contexts. In Nigeria, as well as many low- and middle-income countries (LMICs), challenges abound, ranging from the lack of region-specific datasets to limited AI infrastructure, low technological literacy among healthcare workers, and critical ethical concerns regarding data use and access (Oladipo et al. 2024). This study emerges at the intersection of these challenges and opportunities. It proposes developing a machine learning-powered system, trained on local data, to aid in the early detection and personalised management of Alzheimer’s disease in Nigeria. This model not only fits our context but also reflects our realities.
Methodology
This research employs a mixed-methods cohort design, recruiting 600 participants: 300 diagnosed with Alzheimer’s disease (AD), 200 healthy controls, and 100 high-risk individuals due to family history, comorbidities, or cognitive symptoms. Participants will be selected from federal teaching hospitals in southwestern Nigeria to ensure diversity in terms of regions, ethnicities, and socioeconomic statuses. The study will collect data to develop machine learning models, including cognitive assessments, neuroimaging data, socio-demographic information, medical history, and functional status.
The AI system will utilise interpretable machine learning algorithms, such as Random Forest and XGBoost, for clinical transparency and managing heterogeneous data (Lundberg et al. 2020). Models will be trained on diverse data, including neuroimaging (MRI/PET), cognitive scores, genomic markers, patient outcomes, and socio-demographics.
Natural language processing (NLP) techniques will extract insights from unstructured clinical records, enabling a deeper understanding of patients’ journeys (Rajkomar et al. 2019). Data preprocessing will involve principal component analysis (PCA) for dimensionality reduction and the k-nearest neighbours algorithm for missing values. Models will be validated using k-fold cross-validation and evaluated based on accuracy, sensitivity, specificity, and the area under the curve (AUC). Qualitative methods, such as semi-structured interviews and focus groups with patients, caregivers, and clinicians, will explore perceptions of AI-based diagnostics and personalised treatment. Thematic analysis will interpret this data, ensuring that cultural sensitivity and human-centred design guide AI model development.
Ethical protocols will adhere to the guidelines of the Nigerian National Health Research Ethics Committee, ensuring informed consent, confidentiality, secure data storage, fairness, and clinician training. Community and clinical stakeholders will be engaged to explore perceptions of AI in healthcare and guide culturally grounded implementation strategies. A pilot deployment in southwestern Nigeria will test the AI model’s real-world effectiveness, usability, and ethical acceptability. To address bias, we will utilise fairness-aware algorithms and a representative dataset that reflects Nigeria’s diverse ethnic, socio-economic, and health profiles. Continuous feedback loops and collaboration with local clinicians will refine the model to reflect the local context. Power dynamics will be mitigated through participatory research, with community engagement sessions enabling patients and providers to co-shape the design and evaluation of AI. Transparency in model operations will further promote trust and inclusivity. Recognising Nigeria’s infrastructural challenges, the AI system will be designed for offline use, with minimal data requirements, and compatibility with low-cost devices, such as tablets. It will function reliably even in the event of power or internet disruptions and will be adapted for local languages, ensuring broader accessibility across Nigeria’s multilingual communities.
Expected outcomes and findings
This study develops a machine learning model to identify Alzheimer’s disease (AD) risk early, aiming for a diagnostic accuracy of over 85% in high-risk groups. This advancement seeks to enhance early diagnosis and clinical outcomes. The AI model will classify AD risk as low, moderate, or high, creating personalised intervention recommendations for care plans. Recommendations will consider each participant’s clinical profile, which may involve pharmacological interventions, neuropsychological rehabilitation, caregiver support, and follow-up schedules. The study will evaluate the AI model’s effectiveness in terms of diagnostic accuracy, treatment precision, usability, and satisfaction among both providers and patients. A comparative analysis will assess the AI model against traditional diagnostic methods in Nigerian healthcare. Preliminary findings suggest that AI-assisted screening will demonstrate higher sensitivity and earlier detection compared to conventional assessments, which rely on cognitive testing and symptom observation. The system will offer predictive insights and explainable decision pathways, fostering clinician trust and adoption.
This study will highlight the challenges of integrating artificial intelligence (AI) into Nigeria’s healthcare system, including clinician training deficiencies, infrastructure constraints, and ethical concerns about bias, privacy, and data sovereignty. It will focus on identifying and mitigating biases in AI, particularly related to overfitting to specific ethnic or socio-economic groups. Methods such as fairness-aware machine learning algorithms and regular audits of model predictions across demographics will be used to promote equitable outcomes. Participatory research, involving consultations with clinicians, patients, caregivers, and policymakers, will ensure that the AI system is contextually relevant. Resource limitations will be addressed by developing a scalable, cost-effective AI solution that operates offline or with minimal internet access, optimised for basic computing systems to ensure usability in resource-constrained environments. Support for major Nigerian languages will enhance accessibility and inclusivity. Cases of null findings, such as no significant advantages of AI over traditional methods in specific subgroups, will be documented and analysed for future AI improvements and recommendations. This framework could serve as a blueprint for AI deployment in other low- and middle-income countries.
Interdisciplinary implications
This study presents a culturally relevant AI model for clinical neuropsychology, neurology, and geriatrics, while providing real-world insights into AI ethics in low-resource settings. It has the potential to shape dementia care policy in Nigeria, update medical and psychology curricula to enhance AI readiness, and foster interdisciplinary collaboration among health and technology experts. Above all, it aims to centre the experiences of older Nigerians, ensuring they are not left behind in the global health innovation race.
Conclusion
This research addresses Alzheimer’s disease in Nigeria and the potential of artificial intelligence in enhancing diagnostic accuracy, speed, and clinical outcomes in AD detection. By integrating technology with ethical data practices and cultural contexts, the study aims to develop a diagnostic model that understands the human experience. It aims to detect Alzheimer’s disease earlier, treat it effectively, and enhance knowledge of the disease in Nigeria for the benefit of the community.
The findings suggest that sensitive, resource-adapted AI models can enhance the early diagnosis and management of Alzheimer’s disease, even in diverse, resource-constrained settings such as Nigeria. It acknowledges limitations, such as limited clinical datasets, unreliable electricity and internet access, and potential biases from AI models trained on non-Nigerian data. Addressing these challenges is crucial for practical application. Theoretically, this work advances models for culturally responsive AI and the ethical use of technology. Practically, it provides a framework for similar neurodegenerative conditions across Africa and low- to middle-income countries.
Recommendations include investing in local data collection to ensure that AI models accurately represent the population, training clinicians in the interpretation and ethical use of AI outputs, developing national policies for equitable AI healthcare deployment, and fostering collaboration among AI developers, healthcare providers, ethicists, and patient communities to support sustainable innovation. With adequate investments and partnerships, AI can effectively support the fight against neurodegenerative diseases. This study lays the groundwork for that vision: one line of code, one patient, one narrative at a time.
Acknowledgments
This research benefits from the encouragement, guidance, and support of my mentors, Ayantola Ayalande and Kauna Malgwi, as well as my colleagues, Damilola Dapherede and Onyinyechi Ossai. I also appreciate the facilitators of the LUNE Two AI Fellowship and the Research Round team, with special thanks to Ololade Faniyi and Habeeb Kolade. I extend special thanks to every participant, health worker, and elder whose data and stories will help shape the future of Alzheimer’s care in Nigeria.
References
Adeloye, D., Auta, A., Ezejimofor, M., Oyedokun, A., Harhay, M. O., Rudan, I., & Chan, K. Y. (2019). Prevalence of dementia in Nigeria: a systematic review of the evidence. Journal of Global Health Reports, 3. https://doi.org/10.29392/joghr.3.e2019014
Elijah Kolawole Oladipo, Stephen Feranmi Adeyemo, Glory Jesudara Oluwasanya, Omotayo Rachael Oyinloye, Olawumi Hezekiah Oyeyiola, Ifeoluwa David Akinrinmade, Olubunmi Ayobami Elutade, Dorcas Olayemi Areo, Islamiyyah Olamide Hamzat, Oluwakemi Deborah Olakanmi, Israel Ifeoluwa Ayanronbi, Akinwumi John Akanmu, Faith Opeoluwa Ajekiigbe, Mary Olawumi Taiwo, Victor Michael Ogunfidodo, Christiana Adewumi Adekunle, Precious Oluwadamilola Adeleke, David Ayo Olubunmi, Precious Ayomide Adeogun, & Emmanuel Oluwagbenga Adejobi. (2024). Impact and Challenges of Artificial Intelligence Integration in the African Health Sector: A Review. Trends in Medical Research, 19(1), 220–235. https://doi.org/10.3923/tmr.2024.220.235
Gupta, R., & Zoya Iftekhar. (2024). Artificial Intelligence for Alzheimer’s Disease Detection: Enhancing Biomarker Analysis and Diagnostic Precision. 25–25. https://doi.org/10.3390/ecsoc-28-20206
Kale, M. B., Wankhede, N. L., Pawar, R. S., Suhas Ballal, Rohit Kumawat, Goswami, M., Khalid, M., Taksande, B. G., Upaganlawar, A. B., Umekar, M. J., Spandana Rajendra Kopalli, & Sushruta Koppula. (2024). AI-Driven Innovations in Alzheimer’s Disease: Integrating Early Diagnosis, Personalized Treatment, and Prognostic Modelling. Ageing Research Reviews, 101, 102497–102497. https://doi.org/10.1016/j.arr.2024.102497
Lundberg, S., & Lee, S.-I. (2017, November 24). A Unified Approach to Interpreting Model Predictions. ArXiv.org. https://doi.org/10.48550/arXiv.1705.07874
Oyinlola, O. (2024). Addressing the challenges of dementia care in Nigeria: A call for a comprehensive national strategy. Public Health Challenges, 3(2). https://doi.org/10.1002/puh2.186
Rajkomar, A., Dean, J., & Kohane, I. (2019). Machine Learning in Medicine. New England Journal of Medicine, 380(14), 1347–1358. https://doi.org/10.1056/nejmra1814259
Rane, N., Choudhary, S., & Rane, J. (2023). Towards Autonomous Healthcare: Integrating Artificial Intelligence (AI) for Personalized Medicine and Disease Prediction. Social Science Research Network. https://doi.org/10.2139/ssrn.4637894
World Health Organisation. (2023). Dementia. World Health Organization; World Health Organization. https://www.who.int/news-room/fact-sheets/detail/dementia